
Why Resorts Should Be Trauma-Informed: The Case for a Trauma Aware Spa
By Fred DeMicco and Irene Macabante
The pandemic brought the issues of death and loss to the forefront for many employers. With nearly one million more Americans dying during the pandemic than otherwise would have been expected, organizations likely have at least some employees dealing with loss (Wall Street Journal, 1/11/22). In addition, adding to the stress and trauma, approximately, 3.5 million workers have left the U.S. workforce since March 2020. About 1.2 million from the hospitality industry, thus creating huge challenges and stressors hospitality businesses. Evidence suggests many of these are leaving our hospitality industry for good. Some reasons why these workers are quitting involve the pressures, stressors, and trauma of work- life balance. When the University of Wisconsin at Milwaukee surveyed its employees last year about how the pandemic was affecting them, the results were stunning: Among the 631 university employees who responded, 73 percent reported having one symptom of post-traumatic stress disorder caused by the pandemic. Nearly 40 percent reported having three or more symptoms.
This is not what one might expect from people who generally have stable jobs and health insurance. The university has published toolkits for faculty members and supervisors to incorporate support and resources into their classrooms and departments, and offered workshops for employees and student leaders to learn about trauma-informed practices. (From What One University Learned About Pandemic Trauma and Its Work Force, Sarah Brown FEBRUARY 15, 2022).
Given today’s socioeconomic climate, combined with the stress brought on by the pandemic, now is the time for resorts with spas to become trauma-sensitive and trauma-informed. This is not another thing to add to a diversity/equity/inclusion list to check off. This is about providing the guest with the safest environment possible in order to heal and to do no harm during the course of it. While bodyworkers should be the first ones to be trauma-aware, everyone who has a hand in creating the programming, deciding what is offered, marketing those offers, guiding the guest towards the best services for their needs, and interacting with those guests should be trauma-aware in some form to create the safe, inclusive environment every spa should have.
“Do you need to forgive someone?”
This was a surprising question to be asked while lying face-down on a massage table during a therapeutic massage session. It was surprising because it was 100% accurate. I had come to the spa for some much-needed self-care and nurturing after going through one of the most traumatic experiences of my life. I have no idea how that event manifested itself during the course of my massage, but it did not escape my therapist who was both extremely intuitive and observant.
I do not know if she was officially trauma-informed as this was almost 10 years ago now, but she was trauma-sensitive in some way nevertheless by asking this question. She recognized that I was exhibiting something to indicate that trauma had taken place and was willing to address it and adjust her process in doing so.
I had never been asked this question ever during a massage before – and have not been asked since. With everything that has happened in the last decade or so in terms of social movements like #METOO and #BlackLivesMatter, and influential people like Oprah Winfrey bringing trauma into the spotlight with her book, “What Happened to You?” – I started to wonder: why aren’t healers and practitioners in our industry more sensitive to trauma? Why are they asking questions and doing the same things over and over that can actually do harm by re-traumatizing?
When a spa or wellness organization does not address the fact that trauma is likely present in seven out of ten of its customers, real harm can take place. Re-traumatization can happen and while that is certainly not the intention, being unaware or ignorant of trauma while we are in this position of power has real and lasting effects. And those are not the effects we want for the people who come to us for care.
What is Trauma?
More people know about trauma now than ever before. Bestselling books like The Body Keeps Score by Bessel Van der Kolk introduced trauma into the mainstream consciousness. Last year Oprah Winfrey released a book co-authored with Dr. Bruce Perry called, “What Happened to You? Conversations on Trauma, Resilience, and Healing,” bringing the topic of trauma to the masses, and helping to understand it in an accessible way.
According to the Substance Abuse and Mental Health Services (SAMHS) Administration:
Individual trauma results from an event, series of events, or set of circumstances that is experienced by an individual as physically or emotionally harmful or life threatening and that has lasting adverse effects on the individual’s functioning and mental, physical, social, emotional, or spiritual well-being.
Trauma is commonly defined as experiencing or witnessing a potentially life-threatening or emotionally overwhelming event such as childhood abuse, natural disaster, combat, sexual assault, or car accident1. Experiencing systemic oppression, such as racism, is also a form of insidious trauma.2 The prevalence of traumatic experiences is very common: 70% of adults in the U.S. have experienced some type of traumatic event at least once in their lives. That is roughly 223.4 million people.3
According to trauma expert Dr. Bruce Perry, despite using the word “trauma” all the time, the psychiatric field still debates how to define it: Is trauma an external event? Is it the way we experience that event? Is it the long-term changes in emotional and physical functioning that follow the event? Dr. Perry defines trauma as “an experience, or pattern of experiences, which impairs the proper functioning of the person’s stress-response system, making it more reactive or sensitive.” So, trauma does not necessarily have to be “big T trauma” (such as abuse, combat, or assault) for the event to impair the proper functioning of the stress-response system.
Many people, particularly those in traditionally under-resourced populations, have repeated exposure to trauma over their lifetime. Demographic and identity group factors, including race, gender, immigration status, and profession (such as soldier or first responder), correlate with a higher risk for trauma exposure. Membership in one or more “in risk” groups generally compound trauma exposure and consequently increases risk for many chronic diseases.4
The CDC estimates that the lifetime costs associated with toxic stress, adversity, and trauma at $124 billion.5 A trauma-informed organization alleviates and reduces these costs. In hospitality, this benefits both teams and guests.

Given that 70% of our clientele have likely experienced some form of trauma and come to us for help with their mental, emotional, and physical well-being, it is imperative we understand trauma at the very minimum so as to do no harm. In an ideal scenario, both the organization and its team members would be trauma-aware or trauma-informed so we can transform our practitioners’ care experience from treaters to healers and ensure that those who have survived trauma can access our services.
Defining Trauma-Specific, Trauma-Sensitive and Trauma-Informed
It is important to distinguish the differences between these terms in order to understand our roles as an organization and as practitioners.
Generally, it is out of scope for spa and wellness organizations to provide trauma-specific services geared towards addressing and healing the roots of trauma. Such specific services include cognitive behavioral therapy, EMDR (Eye Movement Desensitization and Reprocessing), or talk therapy.
Because of the nature of our industry, many of the wellness services we provide have tremendous benefits for trauma survivors, but these are not trauma specific. Bodywork, massage therapy, energy work, hypnotherapy and animal/equine therapy have shown to be extremely effective at reducing pain and/or anxiety caused by trauma.
Trauma-informed care (TIC) involves understanding the impact of violence and victimization on a person’s life and development, then offering care that promotes safety and healing and avoids re-traumatization.
The core principles of a trauma-informed approach to care that are necessary to transform a health care setting are: safety, trustworthiness, choice, collaboration, empowerment, peer support, humility + responsiveness.6
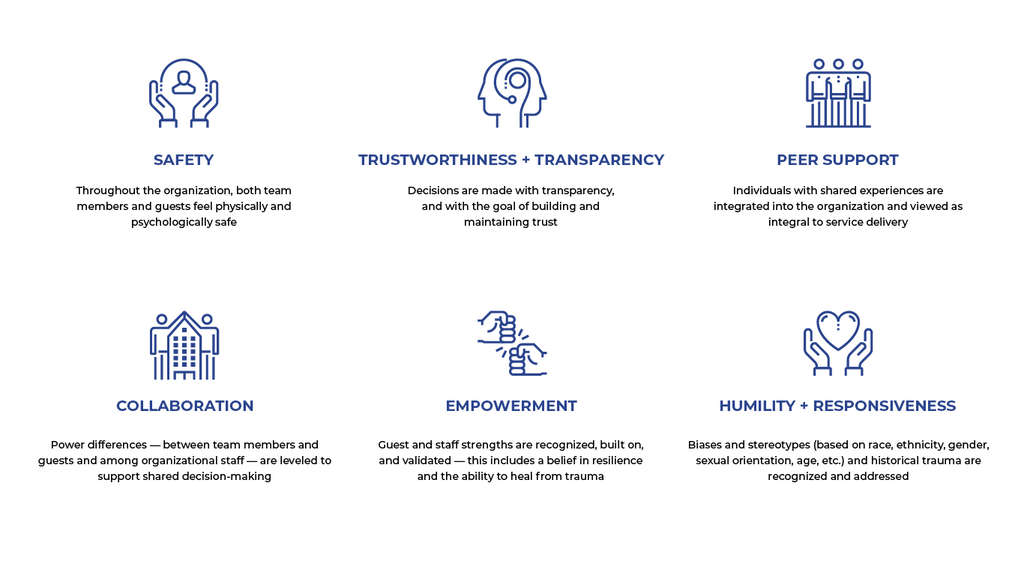
These values are translated into practice through a set of organizational and practical reforms.
Organizational practices include:
- training of both practitioners and client-facing staff
- active engagement of clients in the change process
- and modifying the physical environment
TIC service practices that can be implemented include:
- sensitively screening for trauma exposure
- engaging clients as active partners in their care
- and building referral networks for specialized treatment
It is important to note that TIC does not necessarily involve providing psychological treatment for trauma. It does involve recognizing when unresolved trauma may be impeding a client’s progress and referring them to evidence-based trauma treatment—such as EMDR or cognitive processing therapy—when appropriate.
Trauma-informed care seeks to:
- Realize the widespread impact of trauma and understand paths for recovery
- Recognize the signs and symptoms of trauma in both clients and team members
- Integrate knowledge about trauma into policies, procedures, and practices; and
- Actively avoid re-traumatization.
Not everyone in the organization needs to be trauma-informed, but at the very least, all spa team members should be trauma-sensitive.
Trauma-sensitive means that you become aware of the impact of trauma and how you might see behavior a little differently because of that knowledge.
Let us say a spa receptionist sees someone anxiously pacing back and forth in the lobby or behaving in such a way that looks – on the surface – suspicious. Instead of assuming that they are dangerous or are in the midst of some other negative scenario, a trauma-sensitive team member would think to themselves, “I wonder if they don’t feel safe in our space. I wonder if the spa hasn’t been safe for them in some way in the past.” That is what being trauma-sensitive looks like. It is bringing an awareness of trauma into view and seeing people through the lens of trauma. Note that you do not have to do anything necessarily to be trauma sensitive. In fact, it is better to do nothing than to act on bias.
The Benefits of Trauma-Informed Care in Spa
Think about the many reasons that people visit the spa. While the particulars may be different, at the core, our services provide relief and relaxation for body, mind, and spirit. To do that well, our environments and team members must be sensitive to the guest’s needs and any potential issues or triggers that are counterproductive to relief, rest, relaxation, and recuperation.
Integrating TIC into spa and wellness services would provide important opportunities for us to enhance our understanding of how individuals can truly recover from trauma in body, mind, and spirit. Complementary and alternative modalities offered in spa services — many of which focus on mind–body integration, increasing resilience and regulation, and healthy lifestyle — have enormous potential to expand opportunities to heal from the psychological, physiological, and relational consequences of trauma.

For clients who have trauma in their histories, visiting the spa can be a tricky proposition, especially if they have issues around touch. “Massage therapists are often sought after to reduce pain and anxiety, so a disproportionate number of trauma survivors become bodywork clients. In addition, because touch can be foreign, threatening, reminding of past trauma, or reminiscent of the care received from a parent, massage therapy is inherently more likely to interact with trauma-relevant content than is the case in most professions,” says Mark Olson, PhD, LMT, and director of the Pacific Center for Awareness and Bodywork, which offers a trauma-informed somatic bodywork program in Kaua’i.
As spa and wellness professionals, we understand receiving safe touch has a powerful impact on the nervous system. How can we ensure that this safe touch is available to everyone, especially for those who need it most?
The answer lies in bodyworkers being trauma-informed, having trauma-sensitive team members who can guide clients to the most appropriate services and/or practitioners, and an environment set up to encourage and enhance psychological safety and control. At every stage, there needs to be people who understand, and everybody needs to be on the same page to create that environment.
“If our goal in the spa industry is to help improve people’s mental, emotional, and physical wellness, we have to consider trauma-sensitive or trauma-informed approaches. Otherwise, we think we are delivering a service, but we are really not being effective the way that we can and should be,” says Tiffany Ryan, PhD, MSW, LMT, Yoga Teacher and co-founder of Yomassage, a luxurious and relaxing experience that makes therapeutic touch more accessible.
“Unfortunately, mental health does not play a very big role in our core training as bodyworkers. It’s important to acknowledge our role in the integrated healthcare model and as part of the mental health team.”
Dr. Ryan asserts that spa professionals have a social responsibility to do no harm. “At the minimum, it’s ‘do no harm.’ The maximum is ‘let us really create a therapeutic healing experience for our clients.’ And so, if you look at either end of that spectrum, we have to be trauma-informed.”
A trauma-sensitive spa organization describes a spa environment in which all people – especially those with trauma in their history – feel safe, welcomed, and supported.
A trauma-informed spa organization delivers wellness services in a way that includes an understanding of trauma and an awareness of the impact it can have across settings, services, and the population.
Taking the First Steps: How Trauma-Informed Approaches Can Be Practically Implemented
Taking steps to become trauma-informed start at the organizational level. There are four stages of development in becoming a trauma-informed organization:7
1. TRAUMA-AWARE
Key Tasks: Awareness and Attitudes
Team Members: All
Trauma aware organizations have become aware of how prevalent trauma is and have begun to consider that it might impact their clientele and staff. Most staff:
- know what the term trauma refers to; and
- are aware that knowledge about the impact of trauma can change the way they see (and interact with) others. The impact of trauma is referenced in informal conversations among staff.
2. TRAUMA-SENSITIVE
Key Tasks: Knowledge, Application, and Skill Development
Team Members: All
Trauma-sensitive organizations have begun to:
- explore the principles of trauma-informed care (safety, choice, collaboration, trustworthiness, and empowerment) within their environment and daily work;
- build consensus around the principles;
- consider the implications of adopting the principles within the organization; and
- prepare for change.
3. TRAUMA-RESPONSIVE
Key Tasks: Change and Integration
Team Members: Leaders and Practitioners
Trauma-responsive organizations have begun to change their organizational culture to highlight the role of trauma. At all levels of the organization, staff begins re-thinking the routines and infrastructure of the organization.
4. TRAUMA-INFORMED
Key Task: Leadership
Team Members: Leaders and Practitioners
Trauma-informed organizations have made trauma-responsive practices the organizational norm. The trauma model has become so accepted and so thoroughly embedded that it no longer depends on a few leaders. The organization collaborates with other partners to strengthen collaboration around being trauma informed.
Being trauma-sensitive begins with the intake form, which is extremely important in facilitating the exchange of information necessary to be trauma-aware. Trauma survivors may also be reluctant to, or have difficulty in, verbally expressing what their needs are when it comes to alleviating their PTSD symptoms, so therefore a thorough, thoughtful trauma-informed intake is essential – it gives people another safe opportunity to communicate what they need.

The core intention with TIC should always come from a place of service: how can we create the most therapeutic experience for the client? It might mean having to do some things differently than you normally do to ensure the client feels safe and in control.
The cost to become trauma-aware and trauma-sensitive is negligible, so cost should not be a barrier to implementing these practices in the organization. Companies such as the Traumatic Stress Institute and Trauma Institute International help entire organizations create trauma-informed cultures that increase compassion, resilience, health, and healing. There are costs associated with becoming a Certified Trauma-Informed Organization of course, but the benefits provide a solid ROI: trauma-informed organizations report having greater employee retention, reduced absenteeism, fewer HR-related problems, and increased engagement. For hospitality and spa organizations, guests also benefit from this investment, further increasing the ROI.
Trauma-Informed Bodywork
“Given the pervasiveness of trauma in our society, a massage therapist is going to be more effective with more people if taking a trauma-informed approach. This means realizing what the different forms of trauma are and how they impact the lives of trauma survivors. It means being able to recognize signs of trauma and being skillful in responding effectively to them. It means resisting re-traumatization of trauma survivors. And while a trauma-informed approach is essential for working with trauma survivors, the whole-person approach and the skills associated with it are valuable to apply with all clients,” says Mark Olson, director of Pacific Center for Awareness and Bodywork.

With proper training, massage therapists also learn to recognize what the not-so-obvious signs of trauma are. Oftentimes clients with trauma can come across as demanding, difficult or picky when they are attempting to exercise control over their environment in order to be safe. In addition to some forms of touch, clients may be sensitive to scents or smells, lighting, sounds or music, and set boundaries around these stimuli in order to not get triggered.
In Dr. Tiffany Ryan’s experience, PTSD symptoms such as fight, flight, freeze or fawn have shown up during sessions. “So, somebody is actually advocating for themselves, which is hard to do a lot of the time. And then that may come across as being just a very difficult person. People are anxious. When you are in your sympathetic nervous system mode, when that takes over, you are just trying to protect yourself. And sometimes that might be lashing out, sometimes it might be withdrawing completely and not asking for what you want, at all.” It always comes down to communication – really listening to somebody instead of making assumptions.
For bodyworkers and practitioners, the cost to become a trauma-informed practitioner with CE credits ranges from several hundred dollars to several thousand, depending on the depth and complexity of the course. Both Yomassage and the Pacific Center for Awareness and Bodywork offer trauma-informed bodywork training.
Given the pervasiveness of trauma and its relevance to spa and wellness, we become better-informed spa professionals by becoming trauma-informed. Without the awareness, sensitivity, and proper training to serve those with trauma symptoms, not only are we missing a massive demographic, but we may actually be harming those clients unintentionally when they do come to us for relief. Becoming trauma-informed is an opportunity for us as an industry to provide healing, relief, and a profoundly positive impact for so many people seeking a nervous system reset, whether they are fully aware of it or not. By implementing TIC practices into your company culture, team members are better prepared to work as compassionate peers and be more consistently productive, while providing sensitive and compassionate care for a population of people who need our services the most.
*Acknowledgment: This research sponsored by the GloMed.Education website.
1 Edition F. Diagnostic and statistical manual of mental disorders. Am Psychiatr Assoc 2013:271.
2 Williams MT, Metzger IW, Leins C, et al. Assessing racial trauma within a DSM-5 framework: The UConn Racial/Ethnic Stress & Trauma Survey. Pract Innov 2018; 3:242.
3 The National Council for Mental Wellbeing.
4 A Call to Action: Adoption of Trauma Informed Care in Complementary and Integrative Health Services.
5 Trauma Institute International.
6 Trauma-Informed Care Implementation Resource Center.
7 Adapted from The Missouri Model: A Developmental Framework for Trauma Informed Care, MO Dept. of Mental Health and Partners (2014).



